Health experts push for wider HPV vaccination to cut cervical cancer cases
Globally, cervical cancer is the fourth most common cancer in women, with about 660,000 new cases and 350,000 deaths recorded in 2022. In Uganda, it accounts for an estimated 13 percent of cancer cases among women.
Dr Deogratius Ssenkumba, Medical Officer, Aga Khan University Hospital taking through cancer awareness tips during a media Engagement on Wednesday, May 13, 2026. (Photo by Mpalanyi Ssentongo)
________________
Uganda has been urged to scale up investment in HPV vaccination for adolescent girls as efforts intensify to eliminate cervical cancer by 2030.
Cervical cancer remains one of the deadliest cancers among Ugandan women despite being largely preventable through vaccination and early screening.
Globally, cervical cancer is the fourth most common cancer in women, with about 660,000 new cases and 350,000 deaths recorded in 2022. In Uganda, it accounts for an estimated 13 percent of cancer cases among women.
Dr Deo Ssekumba, a cancer specialist at Aga Khan Teaching University, said the disease is almost entirely linked to the Human Papilloma Virus (HPV), a sexually transmitted infection common among sexually active people.
“The story of cervical cancer often begins with infection during adolescence or early adulthood, but the cancer itself may only appear 10 to 25 years later,” he said during a cancer awareness and media engagement held on Wednesday (May 13) at the Aga Khan University in Nakawa.
Regional disparities
Data from the Uganda Demographic and Health Survey (2022) shows significant regional variation in cervical cancer prevalence.
The Acholi sub-region in northern Uganda records the highest prevalence at 21.4 percent among women aged 15 to 49, nearly double the national average. Lango follows at 20.8 percent, while Kigezi and Kampala stand at 17.3 percent and 17.1 percent respectively. Karamoja (3.4 percent) and Bukedi (6.8 percent) report the lowest prevalence levels.
Diana Ssewanyana, operations manager Aga Khan University hospital, Kampala, addressing journalists during a media engagement on Wednesday, May 13, 2026. (Photo by Mpalanyi Ssentongo)
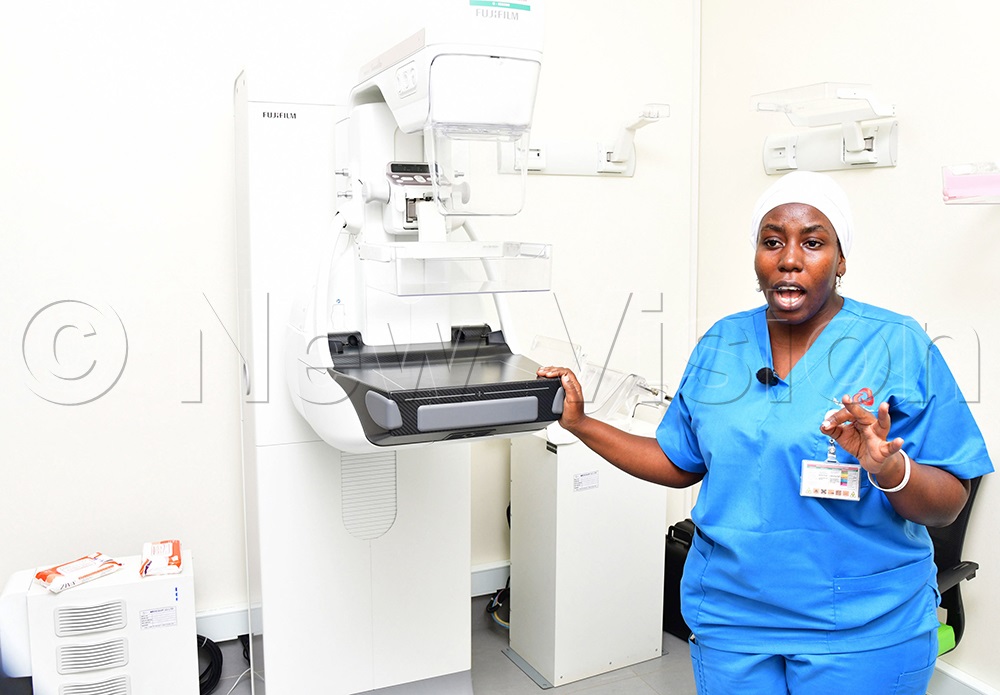
Oncology nurse Kuluthum Ndagire explaining about the mammography machine used for breast cancer testing. This was during a media engagement on cancer awareness and education at Aga Khan hospital on Wednesday, May 13, 2026. (Photo by Mpalanyi Ssentongo)
Vaccination as key prevention tool
Dr Ssekumba said vaccination before sexual debut offers the strongest protection against HPV and significantly reduces the risk of developing cervical cancer later in life.
The push aligns with Uganda’s implementation of the global “90-70-90” strategy aimed at eliminating cervical cancer as a public health threat by 2030. The framework targets 90 percent HPV vaccination coverage among girls by age 15, 70 percent screening coverage, and 90 percent access to treatment for those diagnosed with cervical disease.
He said vaccination remains the cornerstone of the strategy because prevention is far more cost-effective than treatment.
“By vaccinating girls between the ages of 10 and 15, we are stopping the disease before it starts,” he said.
Uganda has already adopted a single-dose HPV vaccine schedule to improve uptake, but Dr Ssekumba warned that misinformation and vaccine hesitancy continue to undermine coverage in some communities.
He urged parents and guardians to ensure girls are vaccinated before exposure to HPV, noting that some studies place the average sexual debut as early as 13 years.
Prevention versus treatment
Dr Ssekumba said the emphasis on vaccination is also driven by the high cost of cancer treatment, particularly for patients diagnosed at advanced stages.
While HPV vaccination can prevent nearly all cervical cancer cases, late-stage treatment often involves expensive chemotherapy, radiotherapy, and surgery that remain out of reach for many families.
He said many patients still report to health facilities at Stage III or IV, when survival chances are significantly lower.
Uganda continues to face major gaps in cancer care, including limited treatment centres, shortages of oncologists, and congestion at the Uganda Cancer Institute.
Private facilities, he noted, are increasingly supplementing public services by offering screening, vaccination, and treatment.
Aga Khan University is also expanding its oncology services, with plans to strengthen diagnostic capacity once its teaching hospital becomes fully operational.
“We have the tools to ensure the next generation of Ugandan women never has to face this disease. It starts with vaccinating every eligible girl,” he said.
Call for coordinated action
Dr Ssekumba said Uganda’s cancer burden remains heavily driven by cervical cancer, which is largely preventable through HPV vaccination.
Although the vaccine is provided free under the national immunisation programme, coverage remains uneven, especially in hard-to-reach areas due to limited awareness, hesitancy, and weak outreach systems.
He called for stronger coordination between government, schools, health workers, and the media to boost awareness and improve vaccine uptake.
According to him, reducing cervical cancer in Uganda will depend more on prevention and early screening than on expanding treatment capacity alone.