HIV/AIDS pandemic lingers despite successes
Uganda's rapid acknowledgment of the crisis and the overarching “ABC” policy, managed to reduce the national HIV prevalence.
UNITED AGAINST HIV/AIDS

In the run-up to World AIDS Day, for the whole of November, Vision Group media platforms are airing and publishing in-depth articles about the disease.
______________________________
By Francis Kagolo
On a good day, Kasensero landing site on Lake Victoria is a hive of activity with fishmongers from as far as Busega, Kampala. Yet the name Kasensero usually brings memories of its dark side in the country's HIV/AIDS story.
It was here in Rakai district, in 1982, that Uganda recorded the first case of a disease that would later become one of the key health and development challenges of our times. It is now 36 years down the road; actors in the anti-HIV/ AIDS campaign are upbeat about the achievements so far recorded.
The country's rapid acknowledgment of the crisis and the overarching "ABC" policy, which consisted of abstinence, being faithful and use of condoms, devised in the late 1980s when infections reached epidemic proportions, managed to reduce the national HIV prevalence.
More than 30% of Ugandans were estimated to have contracted the HIV virus by the late 1980s.
The prevalence rate has since dropped to around 6%. Uganda records about 50,000 new HIV infections annually currently, down from 150,000 in 2013. People dying from AIDS-related illnesses have also reduced by 73%; from 75,000 in the late 1980s and early 1990s, to 20,000 today.
New infections among children have reduced by 86% in the last seven years, thanks to the elimination of mother-to-child HIV transmission (eMTCT) programme the Government started in 2011.
"Our aim of epidemic control (bringing the number of new infections annually below the number of deaths) by 2020 is going to happen," Dr Joshua Musinguzi, the head of the AIDS control programme at the health ministry, said.

People taking a test during an HIV/AIDS awareness campaign. (File photo)
ARVs doing wonders
President Yoweri Museveni is lauded for championing the mass awareness campaign with behavioural change messages like ‘zero grazing' among marrieds that brought down infections in the early 1990s.
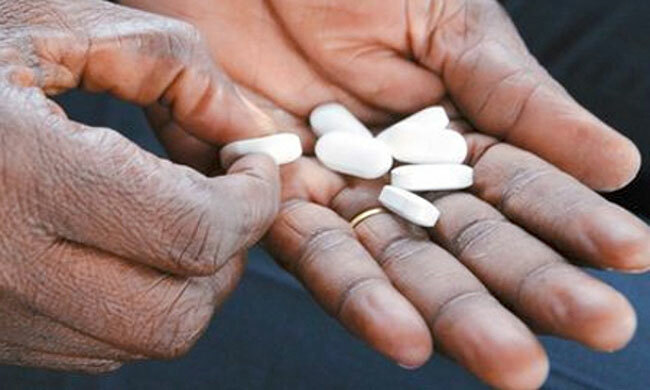
Success has been attributed to access to anti-retroviral treatment (ART/ARVs).
Besides their therapeutic function, ARVs also reduce chances of an infected person transmitting the virus, serving a preventive role too. The 2018 Global Fund report said over 100,000 Ugandans survive catching the virus every year, thanks to ARVs. Uganda rolled out free ARVs in 2007.
In 2016, Government launched an ambitious ‘testand- treat' policy where every person who tests positive is started on ARVs irrespective of their CD4 cell count (level of sickness). As a result, about a million Ugandans of the 1.3 million who are living with HIV are getting ARVs, according to the Ministry of Health.
Dr Musinguzi says ARVs have been a key component in the ministry's combination prevention strategy against HIV.
"It is a combination of ARVs, condoms, PMTCT (prevention of mother-to-child) and other behavioral strategies, including the traditional abstinence and being faithful, which have reduced these incidences," he said.
Not yet Uhuru
But it is not yet time for Uganda to celebrate. James Lule, a project assistant with NAFOPHANU, the national umbrella organisation for people living with HIV (PLHIV) in Uganda, says HIV/ AIDS remains a major health and development challenge.
To control the pandemic, Uganda's target, which is hinged on the global UN 90- 90-90 targets, is to diagnose 90% of all HIV-positive persons, provide antiretroviral therapy (ART) for 90% of those diagnosed, and achieve viral suppression for 90% of those treated by 2020. It is now two years to the 2020 deadline.
"We are implementing the test-andtreat policy but over three million people living with HIV don't get ARVs! Uganda has 40 million people but many have not tested for HIV. We might not achieve the 90-90-90 target," Lule said.
"A total of 4,000 children getting HIV from their mothers is also still a big number. There are intermittent drug stockouts which cause deaths in the long-run. The target is to achieve zero new infections and zero deaths by 2030 but 20,000 people are still dying."
Big challenge
Dr Nelson Musoba, the director general of the Uganda AIDS Commission, said men were slowing the fight against HIV.
"Some men wait for their wives to go for antenatal visits. When the woman's HIV results are negative, the men also think they are negative. But you could be in a discordant relationship," he warned at a recent press conference.
Although fewer men have tested for HIV; more than 51% of the 20,000 deaths recorded last year were men above 15 years. Women deaths stood at 31%, while 18% were children less than 15 years.
"The men are not seeking HIV services and many of them are sleeping with young girls, infecting them with HIV," Dr Musinguzi said.
According to Musinguzi, this explains why over 33% of the 50,000 new HIV infections recorded every year are in girls and young women aged 15-24 years.
Co-infections up

Syphilis is more common among expectant mothers
Experts are worried over the high syphilis and TB infections among people living with HIV, which complicates response to treatment. It is estimated that at least 27% of TB patients are also HIV positive.
Syphilis is more common among expectant mothers and without proper treatment, the disease has diverse effects on the lives of both the mother and unborn baby.
Dr Linda Nabitaka, the Ministry of Health PMTCT coordinator, says that the prevalence of syphilis among women with HIV ranges between 2.5% and 17%, and since both HIV/AIDS and syphilis are sexually transmitted, co-infections and the chances of passing on syphilis are also high.
Way forward
The Conflict, Security and Development Group at King's College, London, recently warned that HIV/AIDS posed a major security risk to Uganda after it was discovered that nearly a quarter of the national army is infected with HIV.
Prof. Vinand Nantulya, the former chairperson Uganda AIDS Commission, says funding remains the missing link in Uganda's HIV/AIDS response. The funding gap for HIV/AIDS interventions stood at $415m (sh1.5 trillion) last year.
"Almost 80% of funding is from development partners. What if it stops? And the fact is that it is beginning to decline. We need to mobilise domestic resources to support the HIV response," Nantulya said.
______________________________
We have a duty to teach people about HIV, says Kabushenga
By John Agaba & Gerald Tenywa
Vision Group chief executive Robert Kabushenga has said the media has a responsibility to educate masses regarding dangers of complacency in the fight against HIV.
"Some people have forgotten that HIV is still with us and without a cure. It is our responsibility to remind them to stay in line," he said.
Kabushenga also encouraged young persons to play their role in averting new HIV infections, which stand at about 50,000 in the country. He said a number of people had forgotten the other ‘face' of HIV, where persons with the virus suffered skin rashes, developed herpes zoster and became thin.
He said it is "important we don't forget where we have come from" in the fight against the disease. There is concern that a number of young women are more afraid of conceiving than contracting HIV when they engage in risky sexual behaviour.
Kabushenga challenged the media to enlighten young people who were born with HIV and were presently sexually active.
"How can we, the media, help them to cope?"

Kabushenga calls on Ugandans to play their part in the fight against the HIV/AIDS
The articles by Vision Group will try to focus on retelling experiences with HIV in the 1990s, when it ravaged the country. "Some of our young people did not witness these experiences, but they are a part of our history in the fight against HIV and we need to appreciate them if we are to defeat the disease," said Kabushenga.
He called on all Ugandans to be responsible and to play their part in the fight against the disease. This, he said, would help those who do not have the virus not to contract it, and those with it to live positively and not infect others.
Lillian Namusoke Magezi, the New Vision health editor, said HIV/AIDS in the country had taken a "new face" which called for a concerted effort.
"Our series will put a historical perspective to the scourge and encourage Ugandans to know their sero status. If you test positive, go for medication. If negative, stay healthy," she said.
Namusoke said the daily stories would empower readers with required information to stay safe and improve the quality of life and take precautionary measures.
Bukedde TV manager Moses Kasasa said all local programmes would have segments on HIV/AIDS effective Thursday.
He said the TV would air profiles of people who have taken the lead in the fi ght against the scourge. "Places like Lukaya, Nakibizzi, Kasensero, Rakai, Naluweerere and Mbiko, which were mostly affected by HIV/AIDS, will be profiled," he said. Uganda's HIV prevalence dropped to 6% from 7.3% fi ve years ago.
However, the country and Ugandans cannot afford to roll their sleeves yet because there is no cure for the disease yet.