HIV+ people embrace new strategy to end HIV/AIDS
People living with HIV believe that the new strategy, whose rollout is expected to begin in September 2017, is a timely intervention.
PIC: HIV activists and CSOs put their heads together to discuss the implementation of the DSDM model during a national level stakeholders' meeeting recently. (Credit: Elvis Basudde)
HEALTH
People living with HIV, together with Civil Society Organizations (CSOs), have hailed the new strategy to end HIV/AIDS by 2020, saying that if rolled out it will go a long way to maintain the quality, care and treatment for all vis a vis the increasing number of clients who are being rolled on treatment.
At a press conference held in Kampala, people living with HIV believe that the new strategy dubbed 'Differentiated Services Delivery Models (DSDM)', whose rollout is expected to begin in September 2017, is a timely intervention.
Differentiated care, or differentiated service delivery, has been defined as, "a client-centered approach that simplifies and adapts HIV services across the cascade, in ways that both serve the needs of people living with HIV better and reduce unnecessary burdens on the health system."
The differentiated service delivery model will address some of the critical issues that are affecting the country's health facility, for example, the overflowing of the health facilities with clients, coupled with the healthcare workforce which has not yet increased.
Lillian Mworeko, executive director of International Community of Women Living with HIV Eastern Africa (ICWEA), said CSOs and service beneficiaries are embracing the strategy.
The strategy's goal is to improve the quality, accessibility and availability of health and social services at national and sub-national level by fostering citizens' demand and enhancing the capacity of community-based organizations to advocate for improved responsiveness and accountability by decision-makers and service providers.
Lately, Uganda has embraced new strategies for ending HIV/AIDS ending HIV/AIDS by 2020.
The Uganda National Consolidated HIV Prevention, Care and Treatment Guidelines 2016, recommend ‘Test and Treat' for all people living with HIV (PLHIV) regardless of clinical stage or CD4 as a critical strategy to enable Uganda to achieve the UNAIDS 90-90-90 goal.
By 2020, 90% of all people living with HIV will know their HIV status, 90% of all people with diagnosed HIV infection will receive sustained antiretroviral therapy and 90% of all people receiving antiretroviral therapy will have viral suppression.
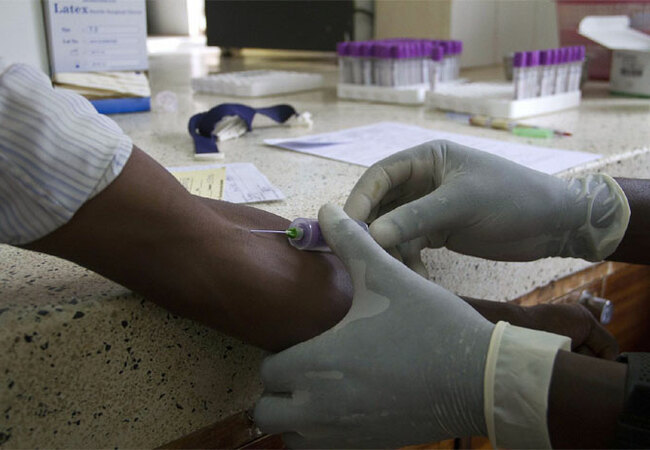
In the same guidelines, Uganda has also adopted Differentiated Services Delivery Models for HIV Testing Services (HTS) and care and treatment.
Under Differentiated Services Delivery, the health systems shift away from "one-size-fits-all" to focus on clients' needs and priorities. Uganda has developed guidelines and has a rollout plan for implementation of Differentiated Services Delivery Models for HIV Testing Services and care and treatment.
This policy shift, according to Mworeko, will affect the different stakeholders including service recipients in different ways much as implementation requires categorization of clients as either "stable or unstable". Proper implementation of the Differentiated Services Delivery Models for HIV Testing Services, care and treatment requires input/contribution from a variety of stakeholders.
The International Community of Women Living with HIV Eastern Africa (ICWEA) supported by USAID/PATH- Advocacy for Better Health (ABH) Project organized a national level stakeholders' meeting to discuss the implications of the model, critic the proposed implementation approaches as well as propose suggestions for better implementation of the Differentiated Services Delivery Models for HIV Testing Services and care and treatment.
The meeting brought together representatives of constituencies and key special groups that are likely to be highly impacted by the changes in the service delivery models of HIV prevention, care and treatment. The Elizabeth Glaser Pediatric AIDS Foundation (EGPAF), which technically supports the Ministry of Health to rollout the DSDM, was also represented.
The content and rollout plan for Differentiated Services Delivery Models (DSDM) for HIV Testing Services, Care and treatment was presented during the meeting, followed by a discussion of the potential shortcomings of the model and then strategies for better implementation of the model were recommended.
ICWEA and EGPAF provided background information of the Models and explained that Models is broken down into differentiated HIV testing services and differentiated HIV care and treatment services through both facility and community based models.
Mworeko said that facility and community based testing for HIV is currently taking place as provider/health worker initiated but the Models will add client initiated testing component. The community based Models for HIV Testing Services will include door-to-door testing, outreach in schools and workplaces, and moonlight testing.
According to Jude Thaddeus Bigirwenkya, advocacy and community empowerment officer, USAID/PATH-Advocacy for Better Health, the Differentiated Services Delivery Models aims to create modifications in client flow, schedules and location to make it easier for these unstable patients in need of extra attention to transition to stability.
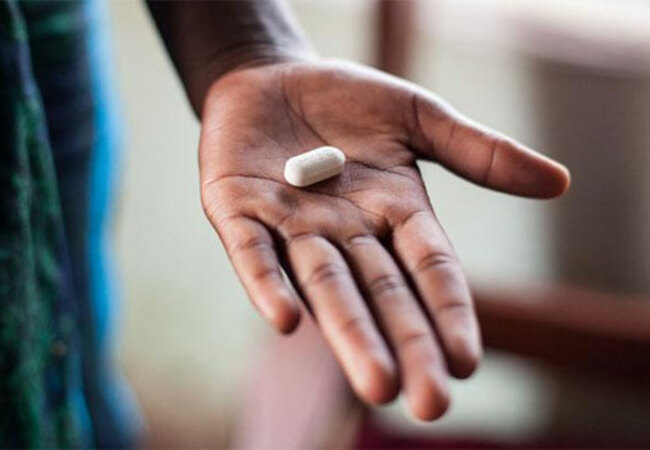
Bigirwenkya says that the community based treatment model is aimed at stable clients included in the Community Client Led ART Delivery Model (CCLAD) or the Community Drug Distribution (CDD).

HIV activists and CSOs put their heads together to discuss the implementation of the DSDM model. (Credit: Elvis Basudde)
The CCLAD creates a community of stable ART clients in order to reduce stigma and create a sense of accountability. A CCLAD group will have one member to pick up medication for all members, rotating so that each individual will visit the facility for testing two or three times a year. The CDD will offer a distribution of medication once a month for 10-15 clients to pick up from local facilities such as schools or easy to access sub-county locations.
CSO representatives were engaged in an interactive discussion addressing three major questions i.e. foreseeable challenges in implementation of the Differentiated Services Delivery Models, how special interest groups ( sex workers, adolescent girls and young women, and IDUs) would fit into the model, and how the key population CSOs could be involved in the implementation of the model.
The challenges identified included:
1. We are still experiencing cases of inadequate health care providers to provide services at the health facilities and conduct community level follow up; how will the Differentiated Services Delivery Models which require more health care workers be handled
2. How will the government sustain this Differentiated Services Delivery Models amidst current issues of drug stock-outs among others in the HIV response
3. How will human rights concerns be handled considering the fact that the Differentiated Services Delivery Models might have space for breach of confidentiality
4. Sex workers are fearing that they might lose customers/clients in case they are forcefully transitioned to access services from their communities
5. There is perceived internal and external stigma and discrimination fueled by the legal environment (especially for all KPs). There is need to focus on the legal environment for effective implementation of the Differentiated Services Delivery Models.
6. Use of illicit drug criminal as per the laws of Uganda and this will hinder drugs users and injectors from revealing their places of residence to facilitate access to differentiate services at community level.
7. The language used "stable and unstable clients" is stigmatizing and discriminatory
8. Corruption was identified as a concern
9. The model was perceived to be expensive especially when domestic funding for HIV & TB is still low
10. Not sure how pre and post counseling will be handled with HIV self-testing
11. There is anticipated conflict of interest regarding the drug distribution points
12. The proposed models including HIV self-testing have no guidelines for operationalizing them
For effective engagement of special interest groups in the implementation of Differentiated Services Delivery Models, meeting participants suggested the following strategies:
1. Identify and mapping "hot spots" which would facilitate effective targeting of key populations
2. Develop a security plan to prevent violence targeting the key populations
3. Heavily invest in community structures to implement the differentiated services at community level
4. Use multilingual documents while training health service providers on the health needs of special interest groups
5. Hold regular dialogues between service users and service providers
6. Sensitize health service providers on the health needs of special interest groups
7. Carry out refresher trainings for different stakeholders e.g. VHTs, CDDP leaders and CLAD leaders
8. Develop a bridged charter which spells out the roles and responsibility of clients and/or patients
9. Install a toll free help lines, and learn from other countries that have started implementing Differentiated Services Delivery Models.
Finally the participants identified CSOs roles in the implementation process which could include;
Mobilizing and educating communities on the Differentiated Services Delivery Models
Advocate for proper implementation and evaluation of the Differentiated Services Delivery Models