Outdated vaccine supply systems constraining immunisation gains
Uganda’s immunisation program has grown tremendously, from the initial six basic vaccines to 10 antigens.
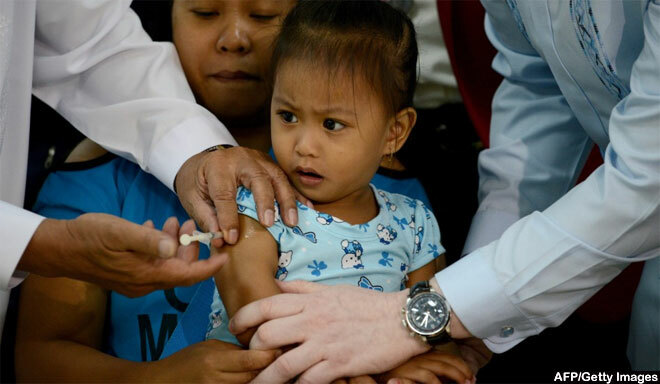
(Photo credit: AFP)
Many new vaccines are coming up quickly; however, vaccine supply and distribution systems are not improving as fast, compromising access to life-saving immunisation and limiting its impact.
This is one of the findings in new research published in the journal Vaccine, released early this month.
Uganda's immunisation program has grown tremendously. From the initial six basic vaccines (diphtheria, whooping cough, tetanus, measles, poliomyelitis and tuberculosis), the number has increased to 10 antigens currently.
In the past three years Uganda introduced three new vaccines -- pneumococcal conjugate vaccine (PCV), human papillomavirus (HPV) vaccine and inactivated polio vaccine (IPV) -- into the routine immunisation schedule.

The country is planning on rolling out three others - rotavirus, measles rubella and Tetanus & Diphtheria by 2018.
"Each new vaccine comes with different requirements," explains Brian Atuhaire, an immunization supply chains expert working with PATH, an international NGO.
"Vaccines are sensitive to temperature. They need to be stored between 2 to 8 degrees Celsius across the whole supply chain from transportation up to the child in the community or they lose potency," he says.
In addition, he explains that every new vaccine requires awareness building. With every new vaccine, there are changes in delivery systems, storage requirements of what would have been a normal process.
Atuhaire also points out changes in ordering and issuing tools that need to be revised, changes in reporting tools making sure they accommodate all the changes.
According to the Effective Vaccine Management (EVM) assessment of 2014, the new vaccines have more than doubled the volume of vaccines that must be tracked, properly stored, and delivered.

The new vaccines are also introduced with more doses and visits required from different age groups and in new service delivery points, such as schools.
"These planned vaccine introductions have nearly tripled the cost of the immunization program from US$31,647,517 in 2011 to an estimated $91,436,221 in 2016," a PATH document, Immunization Supply Chain Policy Environment in Uganda: Landscape Analysis and Advocacy Recommendations states.
It is in this context that the new Vaccine journal findings provide much needed research to inform policy decisions to improve service delivery.
According to researchers, vaccine supply and distribution systems are obsolete and consequently compromise the impact vaccines have on safeguarding people's health.
"We need to apply the same ambitious investments to vaccine delivery as we apply to vaccine development," a release ahead of the journal publication quotes Steve Davis, president and CEO of PATH.
"There are too many places in the world where vaccines are still not reaching the people who need them most," he said.

The World Health Organization (WHO) estimates that vaccines prevent an estimated 2 to 3 million deaths every year.
It is projected that an additional 1.5 million deaths would be avoided if global immunisation coverage improved.
In another study, researchers at John Hopkins University's International Vaccine Access Centre found that immunising children with three crucial vaccines against pneumonia, diarrhoea and meningitis would prevent more than 100 million cases of illness and avert 3.7 million deaths in young children between 2011 and 2020.
However WHO estimates that in 2015, 19.4 million infants worldwide did not receive routine immunisations.
Global immunisation reports indicate that more than 60% of the non-immunized infants live in just ten countries, including Uganda.
The recently released 2016 Uganda Demographic Health Survey report puts average national immunisation rates for all basic vaccines at 55%. However, the Global Vaccine Action Plan (GVAP) recommends coverage of all routine vaccines above 80 per cent.
UDHS 2016 puts the third dose of diphtheria-tetanus-pertussis (DTP3) coverage at 79%, lower than Democratic Republic of Congo at 80%, Kenya at 81%, Tanzania at 97% and Rwanda's 99%.
According to Uganda's administrative data, however, DTP3 coverage is over 95%.
Coverage of the third dose of DPT is often used as a measure for immunisation performance because it indicates completion of the basic infant immunisation schedule at 12 months.
"We must act to close the global immunization gap," says Dr. Matshidiso Moeti, WHO regional director for Africa. "Achieving the Global Vaccine Action Plan goal of universal access to immunisation by 2020 would benefit the health of millions of Africans."

Immunisation makes economic sense
Childhood immunisation is one of the most cost effective public health investments a country can make. Vaccines save lives, prevent illness and disability from immunisable diseases. They contribute to improving children's health and wellbeing and consequently reduce hospitalisation costs. In most cases a cheap, single dose gives lifetime immunity.
IVAC studies estimated savings of $63 billion in treatment and productivity if children in the world's poorest countries were immunised against Hib, pneumococcal and rotavirus between 2011 and 2020 also dubbed as The Decade of Vaccines. According to this study, Uganda could save between $1bn and $10bn in the same period if it achieved immunization coverage of these diseases.
Recent research indicates that every dollar invested in childhood immunisation, returns $16 savings in health care costs, wages and productivity due to illness.
"Immunisation is one of our biggest public health success stories, but safe, effective vaccines don't deliver themselves," a PATH release quote Dr. Orin Levine, director of vaccine delivery at the Bill & Melinda Gates Foundation.
"With consistent, visible support from national and local leaders, every community can have 21st century systems that reliably deliver lifesaving vaccines to everyone who needs them," he says.
Vaccine stock out and storage challenges
The new Vaccine journal is a collection of 29 articles exploring vaccine delivery systems all over the world.
Researchers found that one in three countries in the world experience at least one stock out of at least one vaccine for at least one month.
38% of Sub-Saharan African countries reported national-level stock outs of especially DTP (with HepB and Hib) and BCG.
"When a national level stock out of vaccines occurs, there is an 89% chance that a subnational stock out will occur at district level. More concerning is that if a district level stock out occurs, this will lead to an interruption of vaccination services in 96% of cases," the researchers wrote in one of the journal papers.
"There is a huge move in Uganda to invest in Management Information Systems to provide real-time data to inform decisions. For example with stock outs we should know immediately for quick action," Atuhaire says.
Cold chain equipment failures leading to poor storage temperatures were the other most persistent challenge researchers identified.
For example, an investigation of vaccine equipment failure in Uganda revealed malfunctioning refrigerators, poorly executed preventive maintenance and a lack of corrective action as the root causes.
"The study found that electric-run fridges were being supplied without voltage stabilisers yet power fluctuates all the time," Atuhaire points out.
A simple intervention like improving procurement guidelines to include voltage stabilisers is ensuring cold storage hence maintaining vaccine quality.
To improve vaccine quality, Uganda has phased out sub optimal equipment like gas/kerosene fridges in areas without electricity and bought solar fridges which will help in vaccine storage in every part of the country even where there is no electricity.
The solar refrigerators don't require batteries and store energy in the form of ice, keeping vaccines cool even when the sun isn't shining.
Whereas for now, rigorous temperature monitoring is one of the ways to guarantee that children receive quality vaccines, Dr Robin Nandy the principal advisor and chief of immunisation at UNICEF points out the need to develop vaccines that can better withstand temperature variations.