The plight of Ademu and other teenage mothers
Pregnancy and childbirth complications are the leading causes of death among teenage girls in low income countries
Esther Ademu is a 15-year-old single mother trapped in Ongino-Kumi Hospital following complications of childbirth.
She is stuck because she cannot afford to clear the over sh1m bill for a caesarean section and treatment for sepsis and anaemia, complications she suffered after giving birth at the private hospital five months ago.
But even if the bill is cleared, Esther is stuck because she has nowhere to go.
"For the five months she has been in hospital, we have not seen any of her relatives," says Sr. Luusi Maraka, one of the midwives taking care of her.
A year ago, Esther was living with her boyfriend, a water vendor in Kumi. Unfortunately, he died in a motor accident when she was seven-months pregnant. Esther didn't know the boyfriend's surname or his family.
Her father is alcoholic and she doesn't know where he is. She has never been to school, cannot read and write and doesn't have any skill.
While it is not desirable for anyone to stay in hospital after treatment, in Esther's case, it was perhaps the lesser evil.
Hellen Angolekin and Luusi Maraka, midwives at this private facility as well as other patients' attendants, have watched over Esther and her baby. The two have enjoyed medical attention and support many teenagers who find themselves pregnant would never be able to access in this part of rural Uganda.
Asked whether Esther has been given any postnatal counselling in relation to preventing another teenage pregnancy, Sr. Angolekin told New Vision's Godfrey Ojore.
"We can't start talking to her about it now because her mind is not settled. It is not good to rush her through that information because she is a traumatised girl who lost her boyfriend and went through an operation that she never expected; but once she is set free to leave the hospital we shall take her through that topic."
Sr. Maraka confirmed though, that they have already prepared to address the issue with Esther. The midwives have committed to monitoring her when she leaves hospital so that the baby can complete all the scheduled immunisations.
Teenage pregnancy is common in Uganda. One out of every four girls is pregnant or has had her first baby by the age of 17 and six out of 10 women (59%) that have their first child before age 20.
About 15% (900,000) of 20-49 year old women surveyed were married by the age of 15. 58% of girls 15-19 have experienced physical or sexual violence.
More recent surveys have found that the median age at first marriage for women in Uganda is 19 but the median age for first sex is 16. In contrast, the median age for first use of contraception is 22.7.
This is the road most Ugandan girls take, one that leads many to maternal death or disability when they do not get to healthcare in time. Those who survive the complications may not escape the pain of losing their babies.
"Our people are having their sex at 16 and get Family Planning at 22. There is a lot of discrepancy there," observed Dr Jessica Nsungwa, the Assistant Commissioner, Child health at the Ministry of Health.
Nsungwa was speaking at an advocacy for family planning meeting organised by Global Health Corps for building young family planning champions in Kampala last week.
"Most of the deaths of mothers are among these people. Most premature babies who are dying and costing everybody, costing the government are to these young people. What happened, what went wrong?" she asked.
The Uganda Family Planning Costed Implementation Plan (FP-CIP) 2015-2020, recognises that when teenage girls do not have access to contraceptive information, education, and services, they risk unwanted teenage pregnancy and maternal death.
Pregnancy and childbirth complications are the leading causes of death among teenage girls in low income countries, and this contributes to high rates of maternal death.
Uganda did not meet the Millennium Development Goal to reduce maternal mortality. The country should have brought down the maternal death ratio from 505 deaths per 100,000 live births in 2001, to 131 per 100,000 live births in 2015. However, 2015 World Bank indicators estimate it at 343 deaths, still far from what was set for the MDG target.
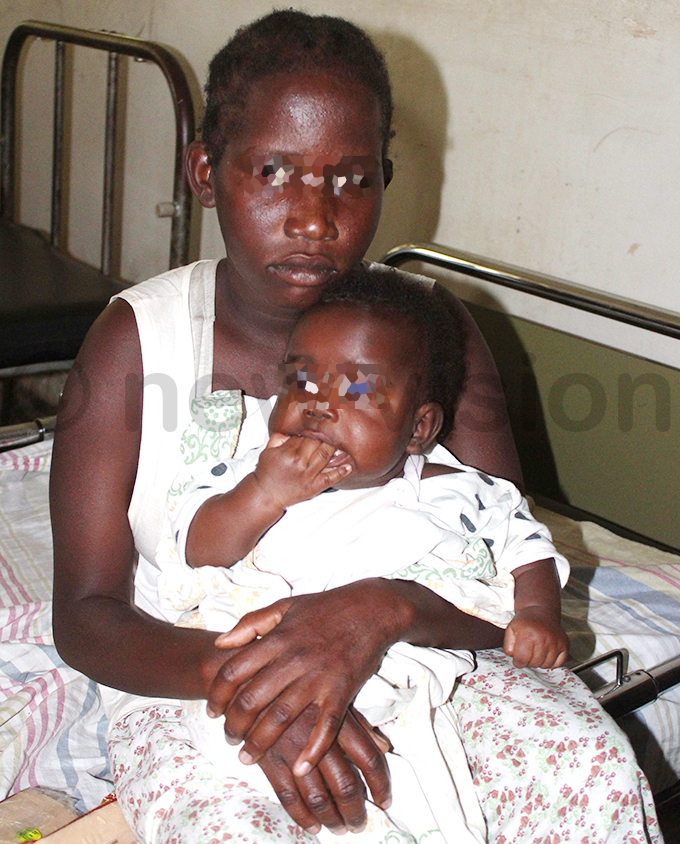 Ademu became a single parent after the father of her child was killed in a road accident. Photo by Godfrey Ojore
Ademu became a single parent after the father of her child was killed in a road accident. Photo by Godfrey Ojore
Family Planning can reduce the numbers of women exposed to risky pregnancies and deliver other socio-economic benefits.
"Family planning is a low cost, high impact intervention and is important if Uganda is to harness the demographic dividend to achieve its Vision 2040 dream to increase per capita GDP from $506 in 2010 to 9,500 in 2040," said Dr Jotham Musinguzi the Director General of the National Population Council who was the chief guest at the meeting.
He explained that family planning can play a role in eliminating the preventable causes of maternal death.
"A high contraceptive prevalence rate is linked to a lower maternal mortality ratio," he told the meeting.
Speaking about global maternal health trends and their implications to Family Planning, Dr Jean Chamberlain Froese, the executive director of Save the Mothers Uganda pointed out that in the developed world 72% of married women use Family Planning and the lifetime risk of maternal death is 1 in 3000.
In contrast, in developing countries, only 34% of married women are using any family planning method and the lifetime of risk of maternal death is 1 in 57.
In Uganda, more than four of every ten births are unintended. Only 26% of married women are using a modern contraceptive while 34% of married women who would like to space the next birth or stop having children are not using a Family Planning method.
The most vulnerable are young people aged 15-24 years. Only 11% of married young people in this age group are using any method of Family Planning.
There are many reasons for this, ranging from a perception that they are not at risk, access to services to myths, misconceptions, fear of or mismanaged side effects.
"The modern woman wants Family Planning with minimal side effects, optimal safety, 100% effectiveness and easily available," Dr Chamberlain said.
She underlined the importance of availability of a wide range of choices for women in improving uptake of services.
"Family Planning methods are like shoes. One size does not fit all. But women have an average of four choices here (Uganda), in Canada we have 15 choices. They (the methods) also need to be available here," she said.
She highlighted the need for forward thinking planning if we are going to meet the needs as a country.
The government has committed to increasing access to modern FP methods targeting a modern contraceptive prevalence rate of 50% by 2020 and reducing the unmet need for FP to 10%.
Among young people, the 2004 National Adolescent Health Policy for Uganda target is to double contraceptive use in sexually active adolescents.
The FP-CIP also highlights the importance of increasing Family Planning information for young people 10-24 years old, as well as creating youth-friendly corners health centres, and adjusting clinic hours to suit the needs of the young people.
It also states as a challenge, the lack of funds for Family Planning services for the youth though government funding for reproductive health commodities significantly increased from less than $1m in 2009/10 to more than $10m in 2013/14.
To increase the number of women using modern contraception from approximately 1.7 million users in 2014 to 3.7 million in 2020, Uganda needs about $39 m every year until 2020.
Dr Carol Sekimpi, the Managing Director Marie Stopes Uganda underscored the importance of generating local resources to fund Family Planning activities.
"Focus of donor-driven work changes according to their priorities. We need local resources to focus on local priorities. Accountability is not just about money, it is about the services offered as well," she said.
The shortage and uneven distribution of healthcare personnel to give Family Planning services also needs to be addressed.
According to the FP-CIP, "the numbers of skilled medical staff are too few in comparison with the need."
Sekimpi tipped on the opportunity presented by the on-going review of the 2012 Ministry of Health- National Policy Guidelines for SRH.
"It provides an opportunity to exploit the Director General's mandate to authorize task sharing," she told the Family Planning advocates' meeting last week.
She explained that task sharing, if approved and implemented can double the number of service providers who even with the same level of investment in terms of staff salaries would be able to provide an additional 8% more services.
This would be a substantial boost to the Family Planning efforts. Already results from PMA2020, a survey monitoring key health indicators every six months, are showing an improvement.
Results shared at the end of August 2016, the fourth round of the survey, show a 4.2% drop in unmet need among married women in the past two years.
The same survey shows a 6.6% increase in uptake of modern contraceptives among married women from 25.6% to 32.2%.
According to the Uganda Demographic Health Survey report, Contraceptive Prevalence Rate (CPR) has been increasing at an average of 5% every five years. By surpassing this trend in two years, current Family Planning efforts may be starting to pay off after all.