Initiative to promote Universal Health Coverage
“We give first aid to those who come and send them to the district hospital."
Every time Jennifer Nantale's team at the Nyaka AIDS Foundation clinic have to send a community member away to find healthcare services elsewhere, she is saddened. Though they would love to reach every one of the people in the Kambuga village community, it would mean the vulnerable orphans and grandmothers the Foundation has pledged to look after could miss out on care.
Nyaka AIDS Foundation set up in one of the remote areas of Western Uganda has a holistic approach to care for HIV/AIDS orphans and their grandmothers but apart from Kambuga hospital which is a ten minute- drive away from the village, there is no other healthcare facility for the population of over 21,000 in the area.
"We give first aid to those who come and send them to the district hospital. It hurts because we know they may not be able to get the services. But if we use our resources on them, we risk using up everything budgeted for the most vulnerable in our care," Nantale, the executive director Nyaka AIDS Foundation says.
She observes that Kambuga hospital can serve many people if only it had adequate resources. To get some services, patients are sometimes asked to meet the cost of fuel to run generators.
The Kambuga community in western Uganda is just one of several hard-to-reach areas in the country where access to effective and affordable healthcare is still a dream. Though, according to Nantale, the people grow a lot of food, they have nowhere to sell it and so do not have cash to pay for other needs like medicines or salt.
According to a World Health Organisation and World Bank Group report, Tracking Universal Health Coverage launched in July last year, 400 million people in the world do not have access to essential health services.

The report found that 6% of the population in 37 of the low and mid-income countries risked slipping back into extreme poverty due to having to make out of pocket payments for health services.
This is a scenario too common for Nantale.
"There was a time our staff got an accident and we rushed them to Kambuga hospital for specialised treatment but we found the hospital needed fuel for the generator in order to run the machines," she says.
"It was expensive for us, an organisation, how about an ordinary person living in Kanungu?" she asked.
To bring attention to such gaps in global health, The Elders, a group of global leaders has launched an initiative to promote Universal Health Coverage.
The third of the 17 Sustainable Development goals launched last year seeks to ensure healthy lives and promote well-being for all by 2030. Apart from achieving universal health coverage, providing safe, effective and affordable vaccines and medicines to all, SDG 3 also commits to ending HIV/AIDS, tuberculosis, malaria and other communicable diseases by 2030.
Governments are obliged to accelerate reforms that ensure everyone, everywhere, can access quality health services without being forced into poverty.
The Elders is an independent group of global leaders and change makers who no longer hold public office but are working together for peace and human rights. The group was first brought together in 2007 by Nelson Mandela former South African president.
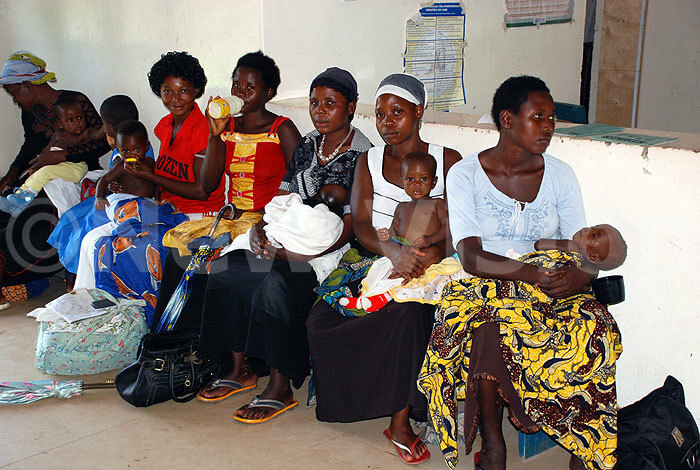
Mothers with their babies waiting for treatment at a health facility in Uganda
Addressing a press conference at the fourth global conference of Women Deliver in Copenhagen last week, Graca Machel, a member of The Elders, called attention to the needs of women, children and adolescents in access to healthcare.
"Women, children and adolescents are more than 60% of the population. The Elders want this group prioritised as one way of meeting the Universal Access to Healthcare goal," Machel said.
She pointed out that the health-related Millennium Development Goals were not met and the reason was that women and children had been forgotten.
"It was not until 2010 when Every Woman Every Child, ten years after the MDGs that there was focus on the groups," she said.
She observed that maternal mortality and infant mortality are high because of internal issues that have not been handled well.
Hina Jilani, another member of The Elders pointed out that despite the availability of free polio vaccination, not everybody was voluntarily taking their children for vaccination because it had become a religious and political issue.
The Pakistani pioneering lawyer and human rights defender decried society apathy towards the health of child brides and the reproductive health complications they suffer.
She pointed out that child marriage in South Asia is the most important human rights issue they are dealing with.
Dr Gro Brundtland (pictured below), the first female prime minister of Norway who is also the deputy chair of The Elders said women and children die because they have no access to life saving interventions.

"Some women get disabled because they had no access to care. Children did or get illnesses that stunt or set them back," she said.
"No one should be denied necessary health services or risk falling into poverty because of medical fees, but this is a reality for hundreds of millions of people across the world," Dr Gro said and emphasised the importance of governments' investments in improving access to health services.
Gro highlighted Sri Lanka's achievement through increased expenditure on universal health which she said has benefited the country.
According to estimates by the World Health Organisation, Sri Lanka's expenditure on health was around 3.2% of Gross Domestic Product or US$89 per head, in 2012. WHO estimate of minimum spending per person per year needed to provide basic, life-saving services is US$44.
Machel called for strong primary healthcare systems, relevant services with qualified health workers where people live.
"Most people in the developing countries are in informal systems and have no access to health insurance," she said.
She observed that where it exists, health insurance in Africa is in the formal workplaces but millions of Africans are not in the formal sector so they are not protected.
"Without a public scheme that provides health insurance, it leaves many vulnerable," she said.
She highlighted the need to look at hidden groups like people with disabilities and link them to universal healthcare services
She pointed out that ordinary people, especially the elderly, were finding it difficult to access care and cope with complicated non communicable diseases.

Graca Machel, a founder member of The Elders at the Women Deliver conference, is displayed on a huge screen
She stressed that universal healthcare was not only for survival, it was a basic right. She argued that it is the responsibility of the public sector and should provide services at all stages of life.
"When you have no children, then what happens to you in old age? You are left as a destitute, especially in the African setting," she said.
From Nantale's observation, even the elderly with children find it difficult to get to care.
"If governments are to offer universal health coverage, it must be a package of so many things," she says.
Apart from expensive medicines, diagnostic services, she points out the challenge of transporting the elderly through bad roads to care.
"It is very rare to find a specialist doctor in the rural districts. Even if you did, they would still be stationed in the urban areas of the regions away from those who need care.
Machel argued that there is often no rationality in politicians' arguments against universal healthcare rather it is an economics issue.
She tipped on the way to get politicians to listen by using the power of numbers, the implication on the economy and making the link to losing power especially at election time because at that moment "they need to bargain."